Your Veins May Be Leaking
 Joseph G. Magnant, MD, FACS, RPVI
Joseph G. Magnant, MD, FACS, RPVI
Venous insufficiency, or leaky veins, is often the underlying cause of many seemingly unrelated symptoms. A simple, noninvasive evaluation by a board-certified vein specialist can expose that hidden culprit.
Carl was suffering with extreme leg pain.
“My legs would tire easily during the day,” describes the 47-year-old physical therapist. “Then, at night, there was a burning sensation with very severe pins-and-needles type tingling. It would get to the point where it would keep me up; I couldn’t sleep. But believe it or not, I had virtually no swelling, bulging, or discoloration.”
Carl sought the help of a podiatrist: “My diagnosis was tarsal tunnel syndrome.”
Tarsal tunnel syndrome is a condition characterized by pain and numbing sensations caused by abnormal pressure on a nerve in the foot. It is similar to carpal tunnel syndrome, which affects the hands and wrists.
The tarsal tunnel is made up of the anklebone on one side and a thick band of fibrous tissue called the flexor retinaculum on the other, forming a tunnel through which several tendons, the tibial nerve, artery, and veins pass through to get to the foot.
“A nerve was actually getting pressed and causing pain and numbness in each of my feet,” recounts Carl. “In order to try to relieve the pressure, they made incisions behind my ankles and performed what they call a retinaculum release, where they cut the retinaculum. During the surgery, they noted that there were huge veins inside the tunnels, but because they did not know how competent the other veins running through my ankles and feet were, they did nothing about them.”
Carl says that initially the pain subsided: “I got complete relief of the symptoms for from four to six months afterward, but as soon as the retinaculum grew back, the pain returned.
“As a physical therapist, I started thinking from a mechanical standpoint: There should be some way to remove the problematic veins from the tunnel. I sought the medical advice of another podiatrist, and he recommended that I see Dr. Magnant.”
Joseph G. Magnant, MD, FACS, is a board-certified vascular surgeon who specializes in vein treatment. His practice, Vein Specialists at Royal Palm Square in Fort Myers, Florida, is 100% dedicated to the modern evaluation and treatment of leg vein disorders.
Venous insufficiency
After examining Carl and reading his medical history, including the op notes from the retinaculum release, Dr. Magnant recommended an ultrasound for Carl to see if there was any venous insufficiency.
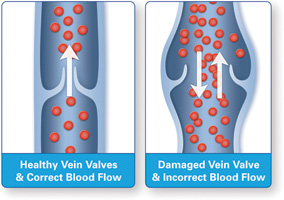
Venous insufficiency is defined as the condition in which the valves of the deep and/or superficial veins of the lower extremities no longer function properly in a one-way manner. These valves are either stuck or scarred in the open position, or are floppy and continue to open, or prolapse, beyond the closed position. This results in reflux or backward blood flow in the veins, which produces increased hydrostatic pressure in the downstream venous system.
Dr. Magnant asked his vascular technologist to perform an ultrasound for Carl. “The ultrasound results showed that Carl had severe venous insufficiency in the great saphenous vein running from the groin to the ankle,” observes the doctor.
“Typically, the normal pressure in healthy veins in which the valves are closing properly is approximately ten millimeters of mercury at the level of the ankle when a patient is standing,” notes Dr. Magnant. “Now, if the valves are leaking from the groin all the way down to the ankle, which Carl’s were, by the end of the day the pressure could have been as high as fifty or sixty millimeters of mercury in that tarsal tunnel. So all of that extra pressure caused fluid to leak out of the vein in the tunnel, as well as causing small veins to start developing within the tunnel. That is why, when the hood of his retinaculum was released, the symptoms were initially relieved. The nerve wasn’t under any more compression.
“However, as scar tissue brought the retinaculum back together, the pressure returned, and because the body heals with inflammation, the pressure was likely higher than before the surgery.”
In order to confirm that venous insufficiency was the cause of Carl’s severe pain, Dr. Magnant first prescribed that he wear compression stocking for three months to see if the numbness improved, which it did. “Based on the good response from the hose, the results of the ultrasound, and the operative findings from the first surgery, I thought it made reasonable sense to seal at least one of the leaking veins, which I did using endovenous closure.”
In endovenous closure, the vein is heated and closed from the inside under local anesthesia using a catheter-based system. The laser systems enable vein specialists to treat patients in the office without anesthesia risks, and patients can return to normal activities immediately.
Defying typical symptoms
Dr. Magnant says he performed endovenous closure on one of the worst of Carl’s two legs: “And because of the significant improvement Carl experienced, we treated his other leg as well.”
“My ultrasound not only diagnosed my venous insufficiency, but it also confirmed how well the other veins in my foot and ankle were functioning,” says Carl. “I only wish we had gone this route before the initial surgery. This is dramatically better than before the surgery. I feel much better.
“As a physical therapist, though, it was interesting to me. I see many patients with venous insufficiency, but their symptoms are typically very different from mine. Usually, we see patients with swollen legs, ulcerations, bulging veins, or skin discoloration.
“I had none of those, so when Dr. Magnant diagnosed venous insufficiency, I thought, Okay, this is going to take some convincing. Then he showed me the ultrasound studies and explained the dynamics of what was happening. Once I understood that, then it made a lot of sense.”
“There are many manifestations of venous insufficiency,” elaborates Dr. Magnant. “Some of our patients experience restless legs or extreme urination frequency at night. Others have ankles so swollen that the calf and ankle appear to have merged as one; my patients often describe them as Grandma’s ankles, piano legs, stovepipe legs, or cankles.
“We recommend that, before patients begin taking diuretics, have a retinaculum release for tarsal tunnel syndrome, go through a urology work up, or are put on medications for restless leg syndrome, they seek an evaluation by a vein specialist to verify there is not an underlying venous insufficiency which may be causing or contributing to the problem. It’s conservative, noninvasive, accurate, and easy to diagnose.”
